Public health challenges in migration and conflict
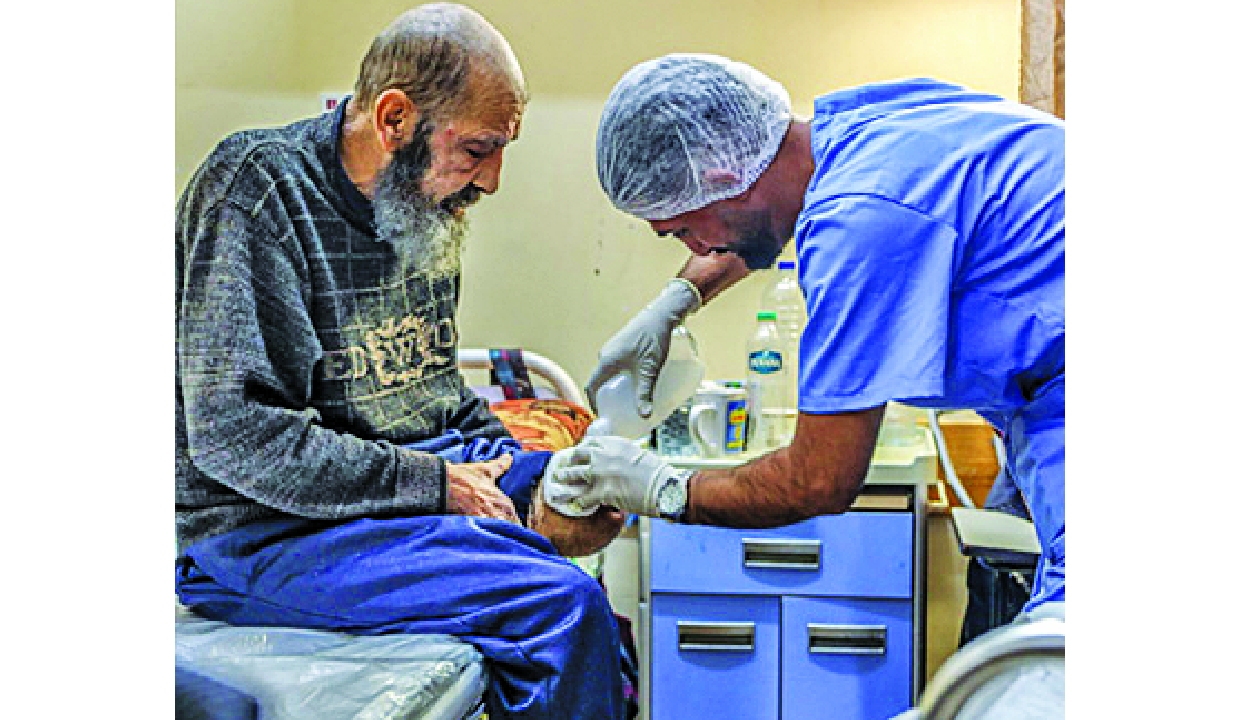
Global health is a shared responsibility among all nations, not the duty of any single country, because no nation exists in complete isolation in today’s interconnected world. This basic concept has been the foundation for ensuring that no one is left behind until today. It has guided international cooperation since the adoption of the Constitution of the World Health Organization in 1948 and led to the development of the International Health Regulations in 1969 and their revision in 2005. This cooperation is reflected in Article 1 of the World Health Assembly in May 1980: “THE WORLD AND ALL ITS PEOPLES HAVE WON FREEDOM FROM SMALLPOX”. Therefore, it was a collective global effort that won the battle against and eradicated smallpox worldwide. However, this concept now appears to be under jeopardy amid the current massive changes in the multilateral world.
The current trend of international negotiations suggests the possibility of emerging threats such as Mpox, a return of COVID-19, and the increasing spread of influenza. These risks require a comprehensive understanding of their underlying mechanisms, cross-national variations, and the available strategies for prevention and mitigation. This cannot be achieved by one country alone; it requires collaboration, trust, knowledge-sharing, and transparency. Such cooperation cannot be sustained through bilateral negotiations that protect one side over the other. This raises the question: have we truly been within a multilateral system, or has it been ruled by bilateral arrangements that continue without fulfilling multilateral obligations? And how will this impact different countries?
There are multiple perspectives regarding the decisions the Trump administration has made since early 2025. They could be seen as a way to direct health priorities, with multilateralism shifting towards bilateral and power-based interests rather than collective global interests, which does not work well in health. They may also highlight a defect that has been eroding multilateral diplomacy for a long time, though this was not very clear before 2025. However, one thing is evident: the growing focus on health security over “health for all” and the broader improvement of the international economy.
In the Middle East and North Africa (MENA) region, many countries are under multiple stressors; many are in conflict or in a fragile state. The sense of possibly being left without support since January 2025 has revealed these countries’ vulnerabilities in terms of public health. In countries such as Yemen and Sudan, all the main aspects of the health system have been depleted because of civil conflicts, and the added weight of losing support has had a major impact. In Yemen, the depleted health system must deal with increased morbidity and mortality caused by the conflict, alongside the spread of communicable diseases, a rising burden of non-communicable diseases, and widespread malnutrition.
The health systems of both countries need to support a huge number of internally displaced persons-over three million in Yemen and over nine million in Sudan. Yemen also acts as a transit country for migrants, which requires additional support from health services. In 2025, over one hundred and fifty thousand migrants passed through the country, with more than 21,500 in December alone, marking an increasing trend in migrant arrivals. These migrants have significant health needs, particularly regarding communicable diseases, which could become a future concern for the government of Yemen and surrounding countries. Prioritising such needs and determining how countries should address them remain critical questions. Irregular migration predisposes both migrants and the local population to increased health risks.
A study by LP Goldsmith on COVID-19 vaccination equity among undocumented migrants highlighted that low vaccination coverage, driven by supply — and demand-related barriers such as limited vaccine availability, documentation requirements, fear of deportation, lack of accessible information, and weak local health systems, further increases public health vulnerabilities in fragile and conflict-affected settings. This represents a serious situation that requires multi-level investment, including strengthening health infrastructure, improving biological disaster preparedness, and building inclusive health systems-all of which demand doubled or even tripled rebuilding efforts in contexts of collapsed governance following civil conflict.
At the same time, countries such as the Kingdom of Saudi Arabia, the UAE, and Qatar may also be at risk of disease spread and may require support. This could influence the emerging shape of multilateral health cooperation. Addressing these issues will involve shifting priorities, especially in light of changing geopolitical interests. Prioritising national health security alone will lead to greater individualism if all countries follow the same approach. This also reinforces the perception that outbreaks originate only in developing countries-an unpredictable and misleading assumption that may further deepen divisions between nations. Many countries are already under extreme political and social tensions. Should we wait until another large-scale global health crisis spreads, and a new wave of widespread mortality leads to the loss of a large percentage of the world’s population, as smallpox once did-killing over 1.4 million annually worldwide in the 1960s-before we regain our solidarity as humans and our sympathy for one another and for the world? Must we wait until then to admit that it is our shared responsibility? Or is this a call to rediscover that same solidarity and unified aim to protect against diseases?
The global landscape is likely to disproportionately affect countries that are already at the bottom of the priority list for support during crises, making them increasingly vulnerable to future disease outbreaks. In the end, will the answer be closing borders? And how will that impact the world? These are questions that must be asked and carefully considered.
Shantesh Kumar Singh, Professor, Centre for International Politics, Organisation and Disarmament, School of International Studies, JNU, New Delhi, India and Weiam Al-Hunaishi, University of Malaya, Kuala Lumpur, Malaysia, Executive Diploma Candidate, United Nations Institute for Training and Research (UNITAR); Views presented are personal.